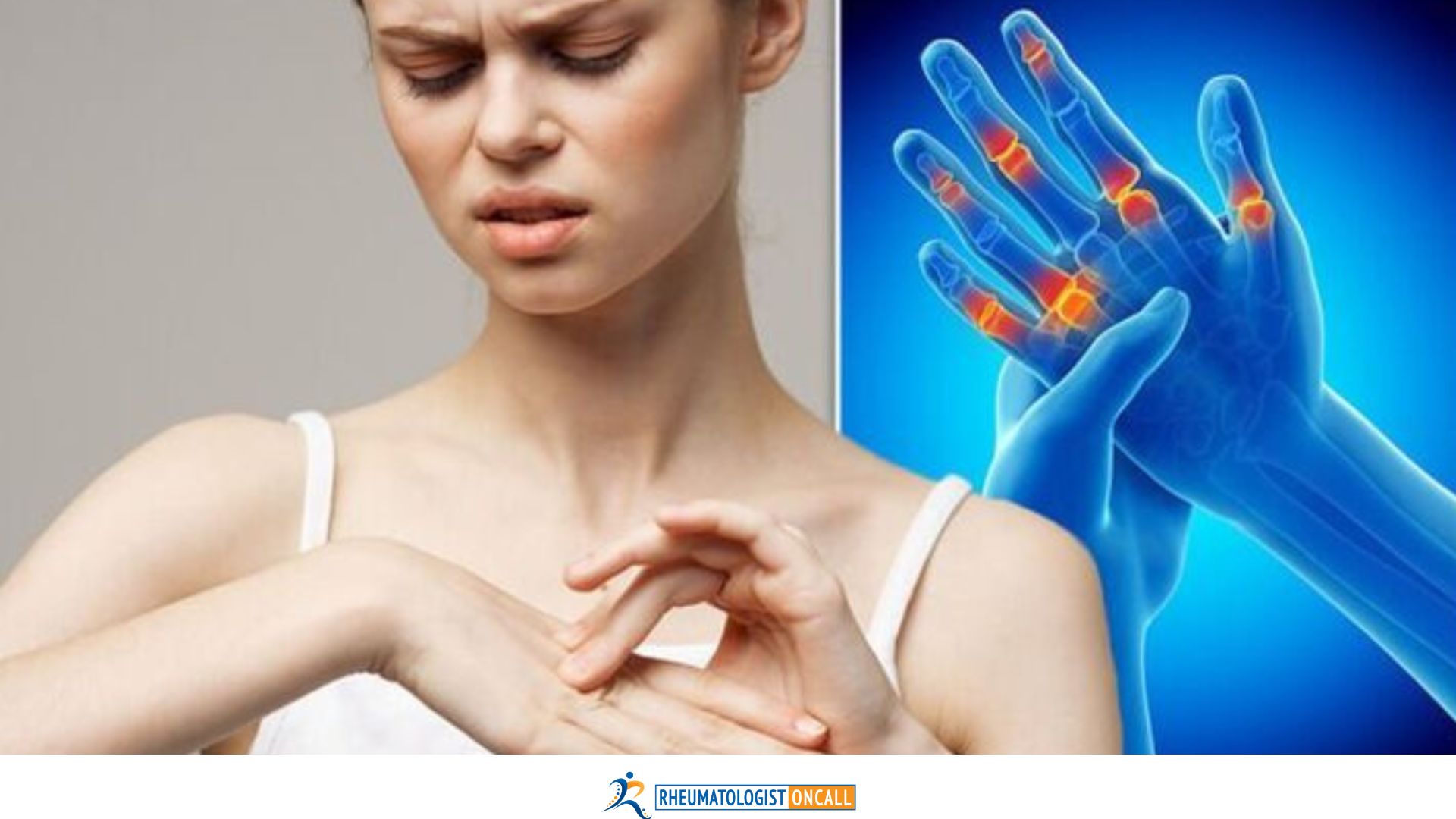
Rheumatoid arthritis (RA) is an inflammatory autoimmune disease. Like many autoimmune diseases, Rheumatoid arthritis (RA) affects three times more women as compared to men.
But why is that?
Why are women more predisposed to develop autoimmune diseases and is there anything that they should be doing to prevent these.
Dr. Diana Girnita, an expert rheumatologist and founder of Rheumatologist OnCall, explains the 5 key reasons why rheumatoid arthritis is more common in females as compared to males.
Having Two X Chromosomes Raises Risk
Females have two X chromosomes while males have one. This matters because the X chromosome contains a gene region called HLA (Human Leukocyte Antigens) that is important for immune system function.
Research showed that there are some certain HLA gene variations that increase the risk for developing rheumatoid arthritis.
Having two copies of the X chromosome versus just one copy means more chance for genetic mutations in the HLA genes to happen in women. Even a single mutation can make someone more prone to getting rheumatoid arthritis.
Shifting Estrogen Levels Impact the Immune System
Estrogen is a steroid hormone that along with impacting sexual function and fertility, it can also regulate inflammation and the immune system, including how your immune system responds to infections. Estrogen works by binding to receptors in cells and plasma and most times has an anti-inflammatory effect, but in certain situations can also cause inflammation. Research suggests that estrogen may regulate the immune response by favoring the survival of forbidden autoreactive clones and ultimately the prevalence of autoimmunity in women.
During a woman’s life, estrogen levels rise and fall with puberty, pregnancy, and menopause. This hormonal flux seems to disrupt normal immune regulation and pathways involved in inflammation.
For example, during prednancy, when the level of estrogen can increase up to 50-60 times, females have less inflammation and their autoimmune symptoms improve significantly.
Later in a woman’s life, after menopause, when level of of estrogen decreases, females may develop more inflammation.
According to Dr. Girnita, these shifting estrogen levels over a woman’s life appear to be an important factor in Rheumatoid Arthritis susceptibility.
Chronic Stress Worsens Autoimmunity

Experiencing frequent stress long-term increases the likelihood of developing rheumatoid arthritis and other autoimmune diseases. “Unfortunately, research clearly shows women tend to have higher stress levels and more anxiety and depression than men,” says Dr. Girnita.
When we experience a lot of stress, hormones like cortisol stay elevated.
This can overstimulate inflammatory immune responses involved in rheumatoid arthritis. Managing stress is especially vital for women to control Rheumatoid Arthritis risk.
Lack of Sleep Causes More Inflammation
Not getting enough deep, quality sleep leads to worse inflammation and increased pain sensitivity – both of which affect rheumatoid arthritis. But studies consistently show women tend to have poorer and more disrupted sleep habits than men.
Dr. Girnita explains, “Factors like childcare duties, hormonal changes, chronic pain conditions, and anxiety impair women’s sleep quality and consistency.” Getting adequate restorative sleep is crucial for women’s health.
Female Immune Cells Produce More Inflammatory Cytokines
Cytokines are proteins that control inflammation and immune cell activity. Research indicates women’s immune cells make more cytokines like interferon-alpha and interleukin-17. These ramp up joint inflammation involved in rheumatoid arthritis.
In contrast, the main male sex hormone testosterone increases anti-inflammatory cytokines. According to Dr. Girnita, this fundamental difference in how female and male immune cells respond makes rheumatoid arthritis more common in females and makes them prone to excessive inflammation.
Tips to prevent the risk of developing Rheumatoid Arthritis in women
Here are some tips to help mitigate the risk of developing rheumatoid arthritis for women:
- Manage stress levels through relaxation techniques like meditation, yoga, or mindfulness. Avoid overwhelming or high-pressure situations when possible.
- Prioritize sleep consistency and quality. Aim for 7-9 hours per night. Maintain good sleep hygiene habits like limiting light and screens before bed.
- Exercise regularly to naturally lower inflammation. Mix in both cardio and strength training.
- Eat an anti-inflammatory diet high in fruits, vegetables, fish, and whole grains. Avoid processed foods.
- Reach and maintain a healthy body weight. Excess fat cells produce inflammatory chemicals.
- Explore hormone balancing options if you have severe PMS or menopause symptoms. Keep estrogen fluctuations in check.
- Avoid cigarette smoke due to its linkage to Rheumatoid Arthritis development. Don’t start smoking and quit if you currently do.
- Limit alcohol which can impair immune function. No more than 1 drink per day maximum.
- Supplement with anti-inflammatory herbs like ginger, turmeric or omega-3 fish oils.
- Stay socially engaged and seek support to combat isolation and depression.
- Get routine medical care and screenings to catch any early signs of autoimmunity.
- Making positive lifestyle choices and managing risk factors where possible can help lower your chances of developing rheumatoid arthritis as a woman. Be proactive about your health.
The Bottom Line
Rheumatoid Arthritis clearly impacts many more women than men, about a 3 to 1 ratio. As Dr. Girnita explains, the main reasons behind this gender difference are women’s two X chromosomes, shifting estrogen levels, high stress, poor sleep, and immune cell behavior. Understanding these gender factors, encompassing why is rheumatoid arthritis more common in females will hopefully lead to better prevention and treatment strategies tailored for female Rheumatoid Arthritis patients.