SHARE
Relapsing polychondritis (RP) is a rare autoimmune condition that can be difficult to diagnose early on. This disorder causes recurrent bouts of inflammation affecting cartilage structures throughout the body. Over time, the cartilage breaks down leading to threatening complications. Identifying key symptoms that should trigger suspicion for Relapsing polychondritis (RP) allows for earlier treatment to limit permanent damage.
This article will overview the ten most common signs of Relapsing polychondritis (RP).
What Parts of the Body Are Impacted by RP Inflammation?
With relapsing polychondritis, essentially any site containing cartilage is vulnerable to inflammation during flare-ups, including:
- Ears
- Nose
- Tracheobronchial tree
- Eyes
- Heart and vessels
- Kidneys
- Joints
- Gastrointestinal system
However, certain locations like the ears and nose tend to be most frequently affected and can serve as important clues pointing to possible RP.
The Variable, Recurring Nature of Symptoms of Relapsing Polychondritis
 One of the defining characteristics of this disorder, and the source of its name, is the waxing/waning, episodic nature of inflammation. Periods of active disease result in clusters of symptoms that may last for several weeks to months. These episodes may be interrupted by variable remission lengths when patients feel relatively normal.
One of the defining characteristics of this disorder, and the source of its name, is the waxing/waning, episodic nature of inflammation. Periods of active disease result in clusters of symptoms that may last for several weeks to months. These episodes may be interrupted by variable remission lengths when patients feel relatively normal.
However, with each recurrence, incremental cartilage injury accumulates. So, over months to years, increasing structural weakness and scar tissue buildup lead to chronic problems like ear cartilage dropping, airway collapse, arthritis, and vision impairment.
Let’s learn about the ten most common signs that should prompt medical evaluation for relapsing polychondritis (RP).
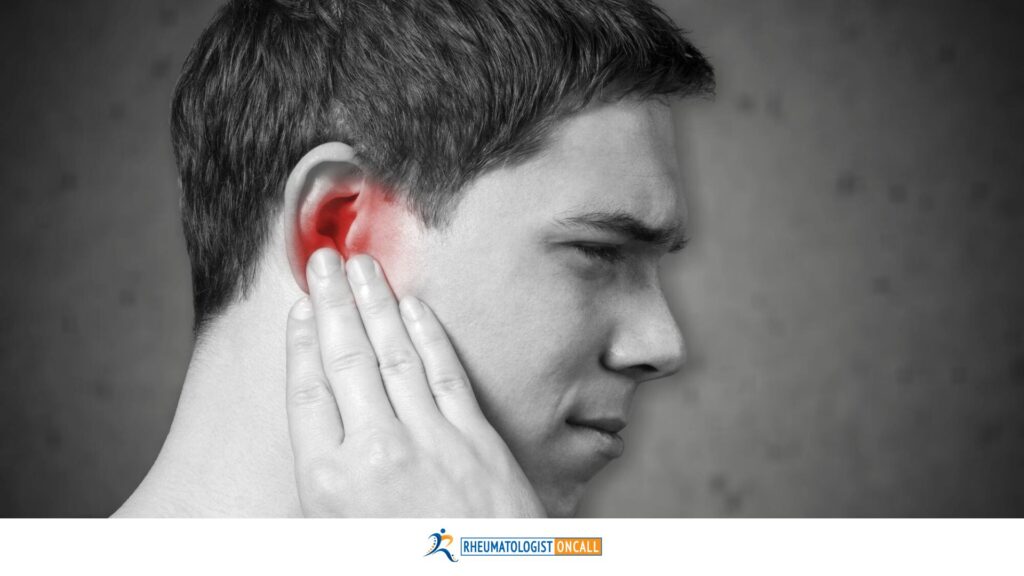
#1: Red, Swollen Ears
While ear inflammation eventually develops in up to 90% of RP patients, it can also be one of the earliest noticeable signs. The initial episode is typically mistaken for an infection, given the rapid onset of warmth, redness, pain, and swelling along the outer ear and antithetical rim.
Key Points About (inflammation of the ear cartilage):
- Usually, it starts unilaterally at first
- It can be quite painful, especially when touched
- Over time, repeated bouts lead to loss of cartilage integrity, causing the ears to become floppy and misshapen (it may look like “cauliflower”)
So when a patient presents with these acute, unilateral ear findings lacking an infectious source, relapsing RP should be considered as a potential cause.
#2: Bridge of Nose Changes
The nasal bridge is also frequently involved (as it contains a lot of cartilaginous tissue) – occurring in around 60% of RP patients. The bridge often looks widened, flattened, or oddly angled, along with pain and local swelling.
Over time, inflammation dissolution of the underlying structural cartilage leads to classic “saddle nose” collapse, where the center of the nose takes on a caved-in appearance from loss of support.
VIDEO https://youtu.be/TfeJoq0CXDY
#3 Inspiratory Stridor
One of the most serious and potentially lethal manifestations of relapsing polychondritis involves the tracheobronchial tree. Repeated inflammation progressively weakens and destroys tracheal ring cartilage. As integrity declines, surrounding floppy tissue can vibrate during breathing – causing loud, high-pitched sounds known as stridor. Typically, stridor begins only with inspiration but becomes constant once tracheomalacia develops.
Attention: Urgent evaluation is warranted when new stridor arises to assess airway patency since RP patients face heightened risks of sudden, catastrophic collapse.
#4: Hoarse, Weak Voice
Given its propensity to affect respiratory structures, RP frequently impacts the laryngeal cartilages, manifesting as changes in voice quality. Hoarseness, vocal fatigue, loss of volume, and pitch control arise as inflammation causes swelling and scarring.
Sometimes, voice alterations emerge early but often develop gradually over time. Thus, newly hoarse patients lacking an infectious source should be evaluated for possible RP.
#5: Costochondritis
While inflammation can theoretically occur in all cartilage types, relapsing polychondritis demonstrates a distinct tendency to involve costal cartilage of the ribs. Repeated flares cause red, exquisitely tender swelling of the costochondral junctions along the rib borders.
Key aspects of RP-related costochondritis:
- Significant pain severity
- Migratory nature – shifts to new rib locations
- Can mimic cardiac ischemia
#6: Joint Swelling and Pain
Over half of RP patients also experience recurrent arthritis flares. The knees, wrists, elbows, and ankles tend to be most frequently involved, but any joints can be impacted.
Distinguishing features of RP joint disease:
- Lack of erosive changes, unlike rheumatoid or psoriatic arthritis
- Tendency to migrate and resolve spontaneously
#7: Eye Inflammation
Eye issues develop at some point in around 60% of RP patients. The spectrum ranges from mild episcleritis to vision-threatening scleritis. Intense pain, photophobia, and eye redness signal significant ocular inflammation that mandates rapid ophthalmologic referral.
Potential eye manifestations:
- Episcleritis
- Anterior scleritis
- Posterior scleritis
- Peripheral ulcerative keratitis
#8: Vestibular Dysfunction
Given its predilection for auricular cartilage damage, RP frequently disrupts inner ear components regulating balance and equilibrium. As a result, true rotational vertigo, lightheadedness, and unsteadiness accompany acute flare-ups.
Sometimes, dizziness and gait instability persist long-term due to permanent vestibular deficits.
#9: Kidney Inflammation
Kidney issues correlate more with generalized systemic inflammation rather than direct renal cartilage damage in RP. Microscopic hematuria and proteinuria coupled with rising creatinine point to possible glomerulonephritis.
Testing for other types of vasculitis (e.g., ANCA vasculitis) along with kidney biopsy helps determine whether secondary small vessel vasculitis drives renal impairment.
#10: Constitutional Symptoms
Similar to other systemic inflammatory diseases, active relapsing polychondritis flares can cause constitutional symptoms like low-grade fevers, fatigue, headaches, and malaise. These systemic manifestations typically accompany acute episodes, causing swollen, tender cartilage at other sites.
Putting Together the Big Picture
As highlighted above, inflammation can crop up virtually anywhere cartilage resides in the body for those suffering from RP. These vague and nonspecific symptoms, coupled with their tendency to recur intermittently, make establishing this diagnosis quite challenging. Hopefully, this article that presents the ten most common manifestations sets the stage for recognizing patterns that should trigger suspicion for Relapsing polychondritis (RP) earlier on.
If you’ve been experiencing painful swelling in cartilage-rich areas like your ears, nose, trachea, or costal joints that tend to come and go, relapsing polychondritis may be the culprit.
Our telemedicine platform at Rheumatologist OnCall provides rapid access to experts in complex autoimmune conditions like RP. We coordinate comprehensive evaluations, laboratory testing, imaging, and specialty referrals to develop personalized care plans for those struggling with unexplained recurrent symptoms. Contact us today to discuss your case in more depth and get connected with an experienced rheumatologist. There is hope!