SHARE
Did you know that the eyes can frequently be affected in patients with ankylosing spondylitis? 25-35 % of patients with ankylosing spondylitis can develop inflammation in their eyes, also called “uveitis”. Often, the inflammation affects one eye, but there are many situations when both eyes are affected. Inflammation of the eyes, uveitis, is a severe complication; you should know about this to get the treatment you need promptly.
In this article, I will discuss:
- What is Ankylosing Spondylitis?
- What are the common signs of uveitis?
- Who is at risk of developing uveitis?
- How do we treat uveitis?
What is ankylosing spondylitis?
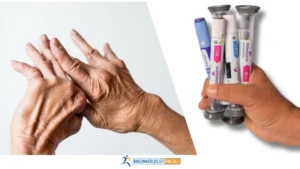
Ankylosing spondylitis (AS) is a common disease affecting about 3.2 million adults in the United States. The numbers can be even higher as many patients get diagnosed later. Ankylosing spondylitis is an inflammatory disease of the back, but it may also involve the joints and tendons in the periphery like your hands, wrists, elbows, knees, or feet. Learn about the most common AS signs and symptoms from my previous blog or watch this Youtube video.
AS affects young adults, usually younger than 45 years of age. Frequently, AS patients experience back or joint pain and severe morning stiffness. The stiffness in the mornings is prolonged-lasting for more than one hour. Moving is helpful and will release joint stiffness.
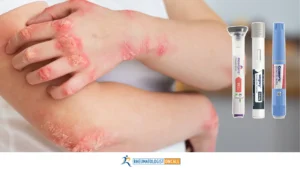
Besides the spine or joints, AS affects other organs like the eyes or the gut. AS affects the eyes in about 25-35% of patients. It may affect one or both eyes.
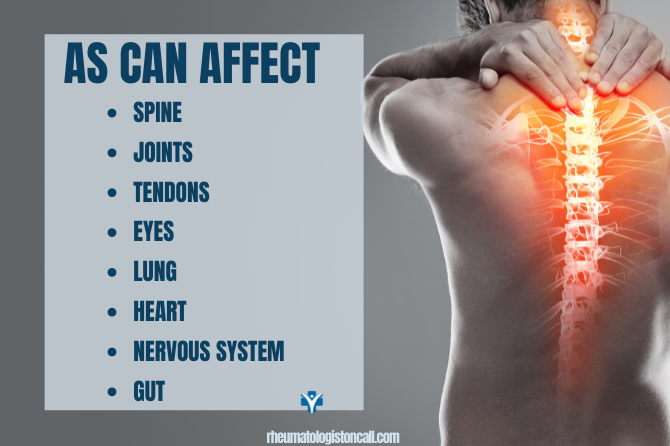
What are the common signs of uveitis?
Patients with inflammation in their eyes will experience:
- REDNESS
- PAIN
- VISUAL CHANGES like blurry vision or photophobia mean patients do not stand the light

These can appear rapidly, and they do require medical attention. If you have AS and experience these symptoms, you should immediately contact an ophthalmologist.
Who is at risk of developing uveitis?
Inflammation of the eye is called “uveitis.” Patients with AS for a long time can develop eye inflammation, and uveitis, at any time. Sometimes uveitis is the symptom that appears before back or joint pain. I have seen patients with a few episodes of uveitis before they start experiencing back pain.
More than that, people with HLA B27 positive have an increased risk of developing “uveitis”. That means that a predisposing genetic factor, like the HLA-B27 gene, will increase the risk of uveitis. If you are interested in learning more about HLA-B27, you can read my blog or watch the Youtube video.
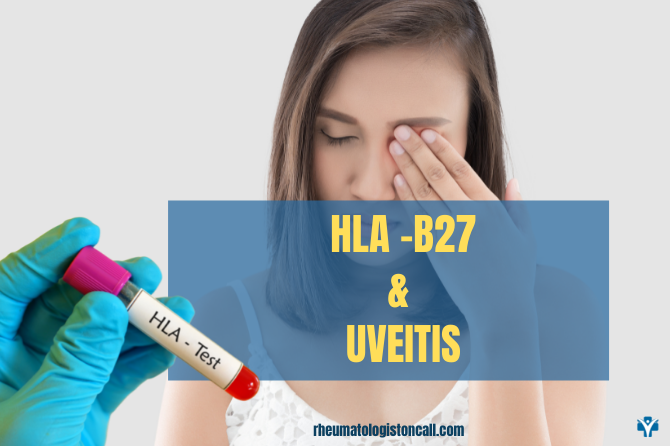
Unfortunately, approximately 50% of people who develop uveitis have AS. The severity of the eye disease is not correlated with the severity of the Ankylosing spondylitis.
How do we treat it?
Uveitis is an EMERGENCY and needs to be treated promptly. Why? It can lead to permanent vision issues like cataracts, glaucoma, or vision loss. How do you treat it?
First, contact an ophthalmologist to evaluate you. Most of the time, for patients with AS, there is close collaboration between the Rheumatologist and your eye specialist.
Second, start treatment. The most common treatments include steroids/ prednisone drops. If uveitis is resistant to local therapy or the therapy with steroid drops becomes prolonged, additional complications such as cataracts or glaucoma can complicate and worsen the situation.
As a rheumatologist, I can contribute to evaluating and starting the patient on systemic therapy. Different systemic treatments like methotrexate, mycophenolate mofetil, or more advanced treatments such as biologics can be implemented. A few years ago, the Federal Drug Administration approved a TNF -alpha inhibitor called adalimumab for treating uveitis.
The patients must continue closely monitoring with both specialists to ensure the eye’s inflammation responds appropriately to the treatments.
If you have developed uveitis that is recurrent or resistant to treatment, or if you have uveitis and you are also concerned about AS, you can consult Rheumatologist OnCall, a telemedicine practice that can evaluate from the comfort of your home. Rheumatologist OnCall broadens access to rheumatology, breaking geographical barriers and being able to help patients in multiple states in the United States. Dr. Diana Girnita integrates the most advanced therapies in rheumatology with a holistic approach that will include lifestyle interventions. Nutrition, stress management, mindfulness, and exercise are essential in achieving lower disease activity and thriving with arthritis. You can contact us if you want a consultation or a second opinion. We are happy to help you!
Contributors to this article:
Diana Girnita MD, PhD and Ana Girnita